Finding the Right Fit: A Guide to Properly Fitting Yourself for a Cane
When it comes to maintaining independence and mobility, a cane can be a valuable tool. Whether you’re recovering from an injury, managing a chronic condition, or simply in need of […]
Finding Relief: How Physical Therapy Can Help Alleviate Sciatica
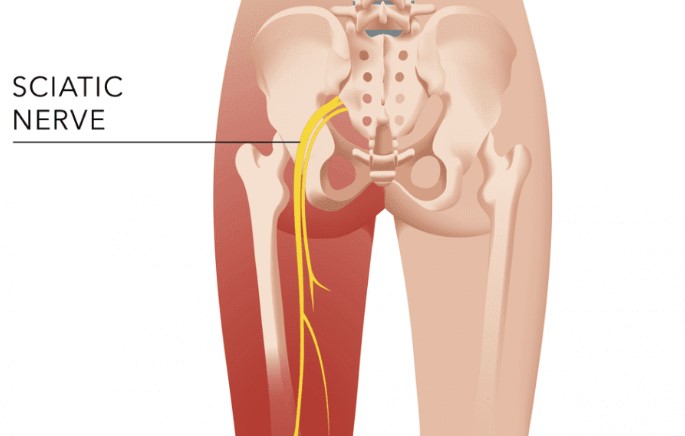
In the intricate network of nerves and muscles that make up the human body, the sciatic nerve is one of the largest and most vital. When it becomes compromised, the […]
Navigating Knee Meniscus Injuries: A Path to Recovery with Physical Therapy

The intricate machinery of our bodies relies on the flawless interplay of joints, tendons, and muscles. Among these essential components, the knee joint stands as a testament to human mobility […]
Hip Osteoarthritis and the Healing Power of Physical Therapy

Introduction When it comes to the intricate mechanisms of the human body, the hip joint undoubtedly takes center stage. This remarkable joint allows us to perform a myriad of movements, […]
Strengthening Your Hips: The Key to Reducing Falls, Preventing Injuries, and Enhancing Overall Health

Hip strength is crucial for maintaining balance, stability, and mobility in our daily lives. While often overlooked, the hip muscles play a significant role in preventing falls, minimizing injuries, and […]
What Is Pediatric Physical Therapy?

Pediatric Physical Therapy: Empowering Children’s Physical Development Children are full of boundless energy and an innate desire to explore the world around them. However, some children may face physical challenges […]
Myofascial Decompression vs. Cupping
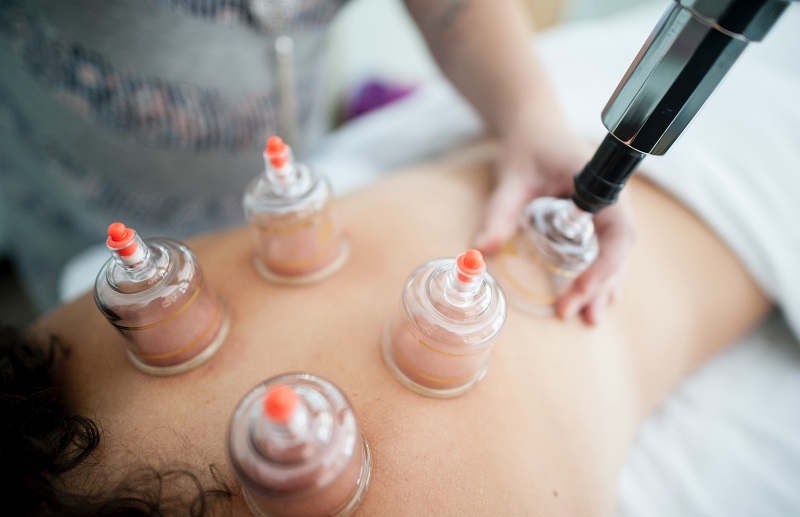
Myofascial decompression (MFD) and cupping are two therapeutic techniques that are often used for manual therapy. This can be performed by anyone from physical therapists to a massage therapists. While […]
Recovering From Rotator Cuff Surgery: What to Expect

Rotator cuff surgery is a common procedure performed to repair a tear in one or more of the rotator cuff tendons in the shoulder. After the surgery, physical therapy is […]
Are You Dealing with Hip Pain?

Lateral Hip Pain and Trochanteric Pain Syndrome By Dr. Maria Suarez, PT, DPT Do you experience pain at the side of your hip? Is it painful when you lay on […]
Does Walking Help If You Have Osteoarthritis (OA)?

By Dr. Caitlin Kenagy PT, DPT What is osteoarthritis? Osteoarthritis (OA) is the most common form of arthritis. It is a term used to describe a breakdown of the protective […]

